Health & Fitness
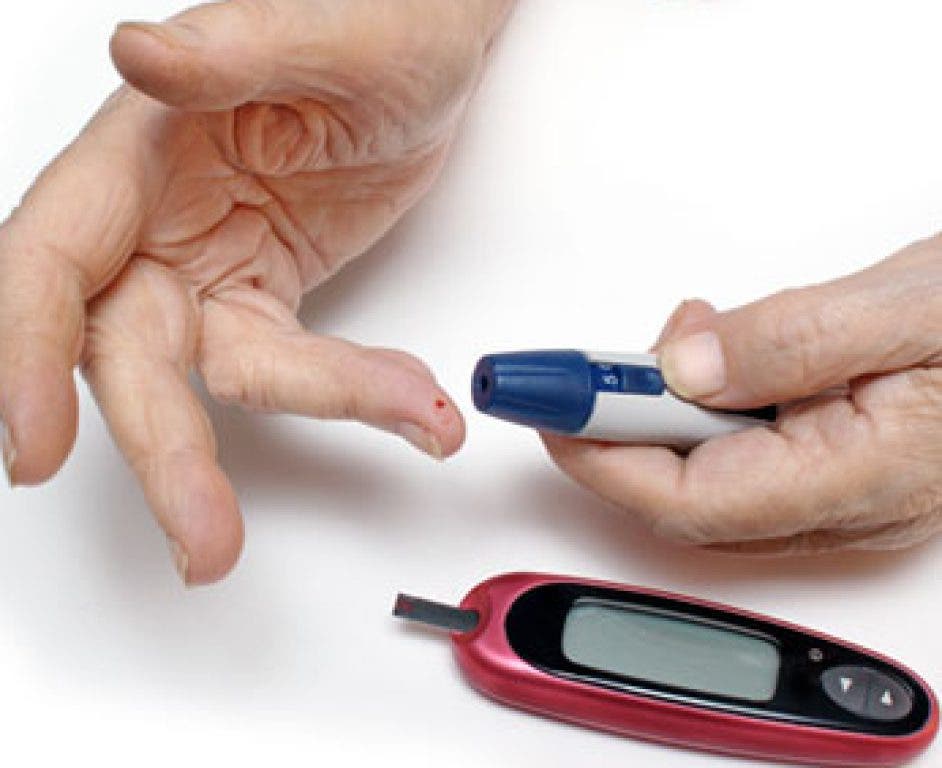
Summertime Safety Tips For Diabetics
It's Summertime! Here, in New England, that means high temps and humidity that can leave just about everyone a little wilted. But folks who are diabetic may have a special challenge.
It’s Summertime! Here, in New England, that means high temps and humidity that can leave just about everyone a little wilted. But folks who are diabetic may have a special challenge. “People with diabetes have an impaired ability to sweat, which predisposes them to heat-related illnesses, as do uncontrollable high blood sugars,” according to Mayo Clinic’s Dr. Adrienne Nassar.
Temperatures of 80°F (about 27°C) or above, especially with humidity, can affect medication, testing supplies, and the health of a diabetic. A diabetic’s body has a harder time handling high heat, combined with humidity (high heat index)
Here are suggestions from CDC’s Division of Diabetes Translation for taking care of yourself during hot weather:
Find out what's happening in Eastonwith free, real-time updates from Patch.
- Heat can affect your blood glucose (sugar) levels and also increase the absorption of some fast-acting insulin, meaning you will need to test your blood glucose more often and perhaps adjust your intake of insulin, food and liquids.
- Drink plenty of fluids, especially water, to avoid dehydration. Avoid sugar-sweetened beverages such as sweet tea and sodas.
- If your doctor has limited how much liquid you can drink, ask what to do during times of high heat.
- Check package inserts with medications to learn when high temperatures can affect them. Take medications with you if you will need to take them while you’re away from home, and protect them from the heat.
- If you’re traveling with insulin, don’t store it in direct sunlight or in a hot car. Keep it in a cooler, but do not place it directly on ice or on a gel pack.
- Check glucose meter and test strip packages for information on use during times of high heat and humidity. Do not leave them in a hot car, by a pool, or on the beach.
- Heat can damage insulin pumps and other equipment. Do not leave the disconnected pump or supplies in the direct sun.
- Get physical activity in air-conditioned areas, or exercise outside early or late in the day, during cooler temperatures.
- Use your air conditioner or go to air-conditioned buildings in your community.
The Joslin Diabetes Center offers these tips for diabetics:
First thing—keep hydrated!! The heat causes you to sweat more and dehydration will raise your blood glucose levels. Water is your best fluid replacement. All good news—no calories, no carbohydrate, and pure hydration. If you do choose fluids with calories, be sure to account for the carbs.
Find out what's happening in Eastonwith free, real-time updates from Patch.
Check the sensation: The heat can fool you into thinking your low. Sweating, flushing, rapid heartbeat these are symptoms of hypoglycemia but they can also be a consequence of the heat. Before you take extra carb you may not need, check your blood glucose. A full glass of water and getting out of the heat may be the answer.
Keep your footwear on: It may be delicious wiggling your toes in the toasty, sun-baked sand, but if you have neuropathy or vascular problems, shoes on. Neuropathy can make it difficult for you to feel if your feet are getting burned. Ditto walking poorly shod on hot pavement. Unnoticed cuts and sores can let bacteria in, leading to a nasty infection.
Take a pump vacation: going to the beach perhaps? The insulin in your pump is just as sensitive to the heat as insulin in a vial. This may be the time to leave the pump at home and carry a pen or vial and syringe in a cool pack.
So be prepared and when you’re in the heat, and keep thinking about all the snow you’re not shoveling.
If you have diabetes and have any questions about coping with heat or other extreme weather conditions, be certain to consult with your medical team. Doolittle Home monitors residents blood sugar to ensure safe glucose levels.